Next to the common cold, an ear infection is the most common childhood illness. In fact, most children have had at least one ear infection by the time they are 3 years old. Most of the time, ear infections clear up without causing any lasting problems. But, if they occur often or are not treated, they can lead to hearing loss or other damage. The American Academy of Pediatrics has written this article to inform parents about the symptoms, treatments, and possible complications of acute otitis media, a common infection of the middle ear.
How do ear infections develop?
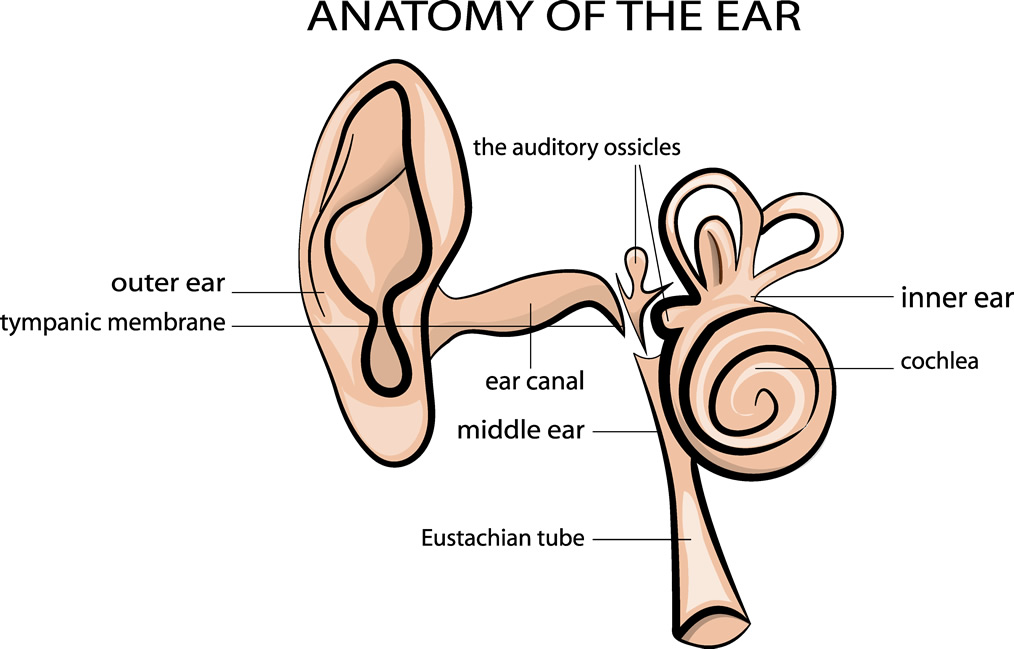
The ear has three main parts – the outer ear, middle ear, and inner ear. A tiny tube, called the eustachian tube, connects the middle ear to the back of the throat and nose. When a child has a cold, nose or throat infection, or allergy, the eustachian tube can become blocked, causing a buildup of fluid in the middle ear. If this fluid becomes infected by a bacteria or a virus, it can cause swelling of the eardrum and pain in the ear. This type of ear infection is called acute otitis media.
Ear infections can develop quickly and often overnight.
Often after the symptoms of acute otitis media clear up, fluid remains in the ear. Acute otitis media then develops into another kind of ear problem called otitis media with effusion. This condition is harder to detect than acute otitis media because, except for the fluid and some hearing loss that is usually mild, there are often no other noticeable symptoms. This fluid often lasts for up to 3 months and, in most cases, disappears on its own. The child’s hearing then returns to normal.
Cross-Section of the Ear
There are several risk factors for developing childhood ear infection.
Age. Infants and young children are more likely to get ear infections. The size and shape of their eustachian tubes make it easier for fluid to build up. Ear infections occur most often in children between 3 months and 3 years of age. Also the younger the child is at the time of the first ear infection, the greater the chance he/she will have repeated infections.
Sex. Although researchers are not sure why, boys have more ear infections than girls.
Heredity. Ear infections can run in families. Children are more likely to have repeated middle-ear infections if a parent or sibling also had repeated ear infections.
Colds/Allergies. Colds often lead to ear infections. Children in group child care settings have a higher chance of passing their colds to each other because they are exposed to more germs and viruses from the other children. Allergies that cause stuffy noses can also lead to ear infections.
Tobacco smoke. Children who breathe in someone else’s tobacco smoke have a higher risk of developing health problems. including ear infections.
Bottle-feeding. Babies who are bottle-fed, especially while they are lying down, get more ear infections than breastfed babies. If you bottle-feed your child, hold his or her head above the stomach level during feedings. This keeps the eustachian tubes from getting blocked.
Parents can help reduce some of the risks of ear infections. For instance:
- Breastfeed instead of bottle-feed. Breastfeeding may decrease the risk of frequent colds and ear infections. If you do bottle-feed, do not give your child a bottle while he or she is lying down in the crib or playpen.
- Keep your child away from tobacco smoke, especially in your home or car.
- Try to keep your child’s hands clean.
Symptoms of an ear infection:
Your child may have a number of symptoms during an ear infection. Knowing what these symptoms are may help you treat some of them more quickly and get medical care, if needed.
Pain. The most common symptom of an ear infection is pain. While older children are able to tell you when their ears hurt, younger children may only appear irritable and cry. This may be more noticeable during feedings because sucking and swallowing may cause painful pressure changes in the middle ear. As a result of this discomfort, your child may have less of an appetite. A child with an ear infection may also have more trouble sleeping because lying down can increase ear pain
There are other reasons besides an ear infection why your child’s ears may hurt. In these cases, your child probably has an earache, not an ear infection.
Ear pain can be caused by:
- an infection of the skin of the ear canal. often called “swimmer’s ear”
- blocked or plugged eustachian tubes from colds or allergies
- a sore throat
- teething or sore gums
Common Illnesses and Conditions
Fever. Another sign of an ear infection is a temperature ranging from 100° to 104° F.
Ear Drainage. You might also notice yellow or white fluid, possibly bloodtinged, draining from your child’s ear. The fluid may have a foul odor and will look different from normal earwax (which is orange-yellow or reddish-brown). Pain and pressure often decrease after this drainage begins but this does not always mean that the infection is going away. If your child needs to travel in an airplane, or wants to swim, contact your pediatrician for specific instructions.
Difficulty hearing. During and after an ear infection, your child may have trouble hearing for several weeks. This occurs because the fluid behind the eardrum gets in the way of sound transmission. This is usually temporary and clears up after the fluid from the middle ear drains away. Because your child can have trouble hearing without other symptoms of an ear infection, watch for the following changes in behavior (especially during or after a cold) that may mean he or she cannot hear well:
- talking softly or in a muffled way
- saying “huh?” or ‘what?” more than usual
- not responding to sounds
- having more trouble understanding language in noisy rooms
- listening with the TV or radio turned up louder than usual
If you think your child may have difficulty hearing, contact your pediatrician. Being able to hear and listen to others talk helps a child learn speech and language. This is especially important during the first few years of life.
Treatment of ear infections
If your child has a fever, ear pain, or shows other symptoms of an ear infection, it is important to see your pediatrician. If your child’s ears are infected, your pediatrician may prescribe an antibiotic. Be sure to follow your pediatrician’s instructions closely. Make sure your child finishes the entire prescription. If you stop the medication too soon, some of the bacteria that caused the ear infection may still be present and cause an infection to start all over again. As the infection starts to clear up, your child might feel a “popping” in the ears. This is a normal sign of healing. Your child’s ear pain and fever should go away within 2 days of starting the antibiotics. Children with ear infections do not need to stay home if they are feeling well, as long as a child care provider or someone at school can give them their medication properly.
Sometimes an ear infection does not go away even after your child takes an antibiotic. If your child still has fever or ear pain for more than 2 days, call your pediatrician. Your pediatrician may need to prescribe a different antibiotic.
To help with pain, your pediatrician may recommend an over-the-counter nonaspirin medicine, such as acetaminophen. Do not give aspirin to your child; it has been associated with Reye syndrome, a disease that affects the liver and brain. Your pediatrician might also suggest putting warm, not hot, compresses against your child’s ears to help relieve pain (This is not recommended for young babies). If your child is old enough to chew gum without swallowing it, give him or her sugarless gum to chew. Have your child sit up as much as possible; this may help lessen pressure on the middle ear and ease pain. An extra pillow at night may also help (Never use pillows in a crib). Avoid using over-the-counter cold medicines (decongestants and antihistamines) as they do not help clear up ear infections.
Complications from untreated ear infections
While your child is young and at higher risk for ear infections, it is important for you to know tile symptoms and to get your child treatment if an infection develops. Although it is very rare, complications from untreated ear infections can develop, including:
- an infection of the inner ear that causes dizziness and imbalance
- (labyrinthitis)
- an infection of the skull behind the ear (mastoiditis)
- an infection of the membranes around the hrilin and spinal cord (meningitis)
- scarring or thickening of the eardrum
- facial paralysis
- permanent hearing loss
The information contained in this publication should not be used as a substitute for the medical care and advice of your pediatrician. There may be variations in treatment that your pediatrician may recommend based on individual facts and circumstances.
Copyright © American Academy of Pediatrics 1996
For more information:
https://www.nidcd.nih.gov/health/ear-infections-children
http://www.kidsgrowth.com/resources/articledetail.cfm?id=1838